A Discussion on Sudden Death and Sudden Cardiovascular Disease
Not long ago, a director of a corporation returned to his seat after a splendid performance on stage during a year-end dinner, only to fell unconscious on the table and never woke up.
Seeing people pass away unexpectedly at their prime, does it make you nervous and ponder: ìWill I be next?î Or do you simply give a sentimental sigh at a sudden and unanticipated death of a young, healthy life.
But, have the bodies of these unfortunate young men really given no warnings at all?
Did you know that having chest pain and chest discomfort may be the way your body is giving you warning signs?! Just as opportunity tends to jump at those who are prepared, luck favors those who tend to their health. Cherish your heart through maintaining healthy lifestyle with good diet habits and regular exercises, to significantly reduce the chance of violent attacks of cardiovascular diseases. People with chronic diseases must pay attention to the maintenance of your body on daily bases, taking your medications on time, to prevent your heart from short circuit.
Written by Chiu-Hua Huang & Ching-Fang Tseng Translated by Danny Lu
Fine a second ago, and dead the next! Lethal accidents always catch people off guard; unforeseen death due to internal causes is even more puzzling and frightening. Sudden death takes thousands of Taiwanesesí lives in their prime annually.
Sudden Death, Who’s Next?
“Sudden Death, by medical defi nition, is when the time from the onset of symptoms to death is less than an hour.î Hualien Tzu Chi Medical Center Cardiology Attending Physician Yu-Chih Chen explains.
Would it be me next?î When Death shows up at your door step, is it really no room for bargain? As news of sudden death occur over and over again, it can be really startling.
Fear is derived from the unknown. Cardiologists encounter sudden death often, and they are no strangers to the cause of it. Because they understand its causes, they remain cautious but have no fear.
Looking back at his medical career from residency training to now a senior attending physician, Dr. Chen has encountered numerous emergent cases. As he speaks of his first sudden death patient, even though it was 11 years ago, he recalls it as it just happened yesterday
ìIt was during my first nightshift in the medical ward as a resident physician. A patient was admitted to the gastroenterology service from the ER. He vomited blood and complained of intense chest pain. The nurse informed me to measure his blood pressure. I remember it was 160/90mmHg, slightly higher than normal. Just as I fi nished the measurement and was about to leave to contact his gastroenterologist, the nurse noticed the patient fell unconscious. She screamed: ëThe patient has no pulse and stopped breathing We rushed to perform resuscitation. The entire event lasted no more than 10 seconds.
Sudden death happen when strolling, when exercising, and even during hospitalization. In late February 2008, Ma Zhao-jun, a music producer, 48, passed out on his way to a shopping mall and was pronounced dead after being rushed to the hospital. It was suspected his sudden death was triggered by a heart attack. Early March, Liao Wei-der, 36, younger brother of news anchor Liao Hsiao-chun, fainted on the basketball court and was soon pronounced dead after arrival at the hospital. He was admitted once for chest distress. Also in Taichung County, a bus driver died suddenly during a 20-second wait at a traffic light. Mid August, a bus driver in Taipei County, not yet 50 years old, experienced intense chest pain. He quickly evacuated the passengers and planned to seek medical attention, but it was already too late.
Statistics shows approximately 300,000 to 400,000 Americans die annually of sudden death. Not counting sudden death in newborns, the peak age of sudden death ranges from 45 to 75 years old and happens one in every thousand people. In Britain, 50,000 people die of sudden death every year. In EuroAmerican countries, the incidence of heart diseases far surpasses that of Taiwan, but it is still estimated that few thousands Taiwanese will die of acute heart diseases every year.
90 percent of sudden death is caused by heart attack. Dr. Chen says.
He emphasized that sudden death as a result of heart attack, in medical terms, is known as ìSudden Cardiac Death (SCD)î. Which heart disease is the most frequent cause of sudden and unexpected death? Acute myocardial infarction is an answer that most would agree with. But in reality, these stealth assassins also include aortic dissection and pulmonary thromboembolism. Majority of the SCD is caused by ìacute myocardial infarction complicated by malignant cardiac arrhythmiasî. In clinical experience, 80 percent of the patients who are admitted to ER due to acute myocardial infarction complicated by cardiac arrhythmias are induced by supraventricular tachycardia.
Heartbeat, Not Too Fast or Too Slow
Cardiac arrhythmias, in laymanís term, means irregular heart rate; heart beats too fast, too slow, or sudden changes of pace, is considered abnormal.
Why does the heart beat ? Cardiologist Jen-Jer Hsieh poses a fundamental question regarding the function of the heart. ìAll of our organs are made of fl esh, so why does only the heart beats?
Perhaps he has explained to his patients few thousand times already, Dr. Hsieh, with a fluent and humorous Taiwanese dialect, provides his own question with a simple answer: Because of electricity! In comparison with internal organs like liver, stomach, and kidney, the heart beats because it has a power plant and a pair of high voltage cables, causing the heart to beat through electrical stimulation and current conduction.î Patients are then enlightened by his straightforward answer!
Specialize in electrophysiology, Dr. Hsieh is adept in Radiofrequency Ablationî (or ìcatheter ablationî) to treat arrhythmia. The engine that beats the heart is concealed in the right atrium, generating electricity just as if a power plant would, and through conducting pathways it stimulates the heart. Under normal circumstances, an individual only has one set of conduction pathways. In the cases of arrhythmia, 80 percent of the patients have ìRe-entry arrhythmiaî, and with appropriate treatment, 90 percent will make a full recovery.
Tachyarrhythmia means the normal and extra conducting pathways in the body short-circuits, leading to rapid heart rate. This happens in approximately onethousandth of the normal population. ìToo many high voltage wires cause shortcircuit, leading to irregular heart beat, and hence arrhythmia.Dr. Hsieh says.
Having alpitations is the main symptom of arrhythmia,î Dr. Hsieh says, But most palpitation are benign.
Patients with arrythmias would first sense palpitations, feel chest discomfort, and seek medical care. EKG is usually done in the E.R. for palpitations. ìBut, arrhythmia is like a child playing hideand-seek. By the time the discomfort is gone, the arrhytmia also hides away.î A sudden attack that quickly self-resolves to normal rhythm is the nature of arrhythmia. To diagnose arrhythmia, cardiologist would ask the patient to carry with them a portable device, providing ìtwenty-four hours of Holter monitoring that records the heart rhythm for an entire day.
If you experience palpitations, you can measure your own pulse. If your heart rate is around 60 to 70 per minute, it is mostly normal. If it is irregular, or as fast as 150 or 160 per minute, or if you have a hard time grasping for air and feeling nauseated.
Or if you measure with a bloodpressure monitor, and the reading of your pulse is around 160, the chance of a cardiac arrhythmia is increased considerably, Dr. Hsieh explains, Then we can proceed directly with electrophysiological study (EPS), and at the same time perform radiofrequency ablation.
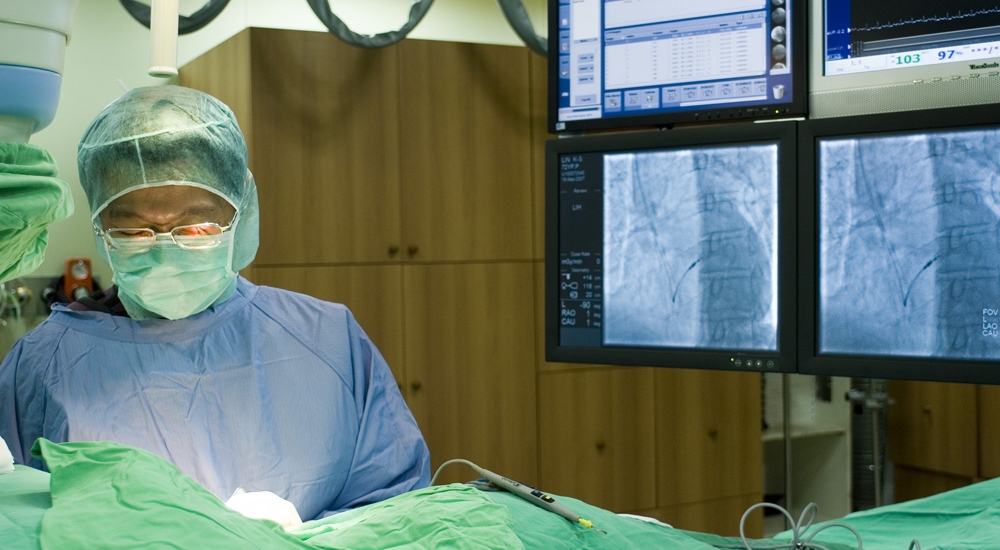
Conducting pathways of the heart is invisible to the naked eyes; it relies on EPS to reveal its presence. The operator executing EPS and treatment requires vigorous training; it must be performed in the cardiac catheterization lab and is considered an invasive surgery.
When asked about the frequency of cases and effects of ablation treatment for cardiac arrhythmia, Dr. Hsieh responds immediately: A lot! Even in our own hospitals many people suffer from arrhrythmia, from custodians to technicians. The average success rate of EPS is 95 percent.
During EPS, ablation is performed to remove extra conducting pathways, and the problem of arrhythmia is solved.
Seek Treatment with Chest Pain or Distress
Inside the waiting area of Cardiac Function Examination Room, gentle music with comfortable displays relaxes the tensed mood; the interior design was done and paid by Dr. Hsieh out of his own pocket.
Proceed further and behind another door, a patient has just completed his electrocardiogram. Grandpa, have you had heart surgery before?Dr. Hsieh asks, looking at the EKG at hand.
No, I havenít.Grandpa answers.
Do you smoke?
Yes, but not as much nowadays.
I canít finish a pack in two days Grandpa is eager to explain his effort in combating his lasting addiction.
After a brief discussion with technician Hsiu-hsiang, Dr. Hsieh turns his head towards the patient,Grandpa, the blood vessels in your heart has been blocked before, causing old injuries!
Michael, I am Hsieh Jen-jer, Mr. Jienís ECG indicates old MI (Myocardial Infarction)ok, and Iíll ask him to go back directly.
After speaking with Dr. Chen Yuchih, a.k.a. Michael, through the phone, Dr. Hsieh confi rms that the patient is unfi t for an exercise electrocardiography, so he asks the patient to return to the clinic for further examination.
Injured blood vessels, how can it be?Grandpa consults the doctor, puzzled about his heart condition.
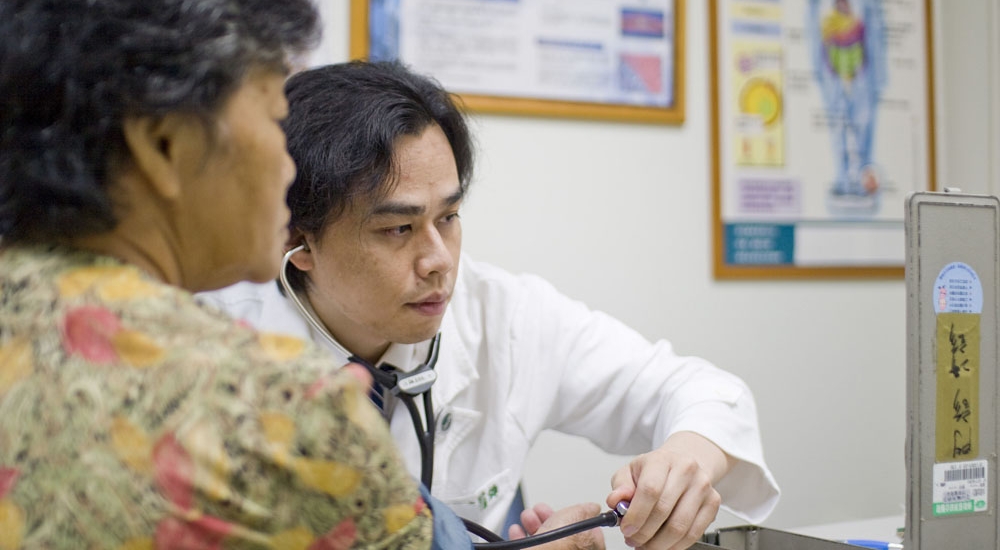
Mr. Jien, not yet in his 70s, came to cardiology due to occasional chest distress and pains. Through a page of static electrocardiogram, the cardiologist accurately determined the conditions of patientís cardiovascular system. The subsequent step would be to inform the patient of the appropriate treatment plan.
Even though Mr. Jien only realized that his heart has already suffered some injury once he came to medical attention, but at least he had minimized the chance of a sudden death!
Avoidance of Sudden Death Through the Window of Opportunity
For the prevention of sudden death, Dr. Chenís first advice is for everyone to learn CPR. Director Hu Sheng-chuan of E.R. has been promoting this vigorously. Dr. Chen says.
If chest distress and pains persist for more than 15 minutes, an ambulance must be called, because this means a possible congestion in the blood vessel, and myocardial infarction may occur! Both Dr. Chen and Dr. Hsieh emphasize that the patient should not operate vehicles on their own, since if they fell unconscious on the way due to arrhythmia, they might cause car accidents, injuring themselves and others.
When malignant cardiac arrhythmia occurs, rapid heart beat cannot effi ciently pump blood to the brain and other vital organs, leading to cerebral hypoxia and organ failure. You have only a 4 minute window to resuscitate and prevent permanent brain damage. Within these 4 minutes CPR must be performed or the heart defi brillated with automated external defibrillator (AED). Dr. Chen points out, international airports, public spaces, and ambulances are all equipped with AED to race against time, to immediately apply cardioversion to convert rhythm back to normal.
Dr. Chen mentions half of his clinic patients complain of chest pains, but the majority of cause is not from blockage of coronary vessels. The causes of chest pains can be as severe as myocardial infarction, aortic dissection, pulmonary thromboembolism, and angina pectoris. However, if one seeks outpatient service upon the onset of symptoms, the recovery rate ranges from 50 percent to 100 percent.
As for myocardial infarction, ìwe must seize the opportunity to treat within 12 hours of the onset of symptoms. If the patient delays medical attention for one or two days, by that time the heart may have suffered irreversible damage and no treatment will be curative.î Dr. Chen, a specialist in interventional cardiology, reminds the patients to be aware of their symptoms.
Relief and Regulate Stresses in Life
Listening to the music played in the Cardiac Function Examination Room, Dr. Hsieh hum with the music and says: ìThe music is played for the patients. Some patients start asking ëwhen is my turní not long after they are seated. People with impatient personality are very susceptible to heart problems!
Though without statistical support, his theory seems logical.
ìWhat about cardiologist?
Oh, we are even more impatient, of course. Otherwise how we can manage as a cardiologist! The music is also for me.î Apparently, while reminding the patients to slow down their pace, cardiologists are also regulating their own pressure.
To stay away from sudden death, donít smoke, develop good habits, do moderate exercises, relief stress regularly, and seek medical attention when symptomatic.